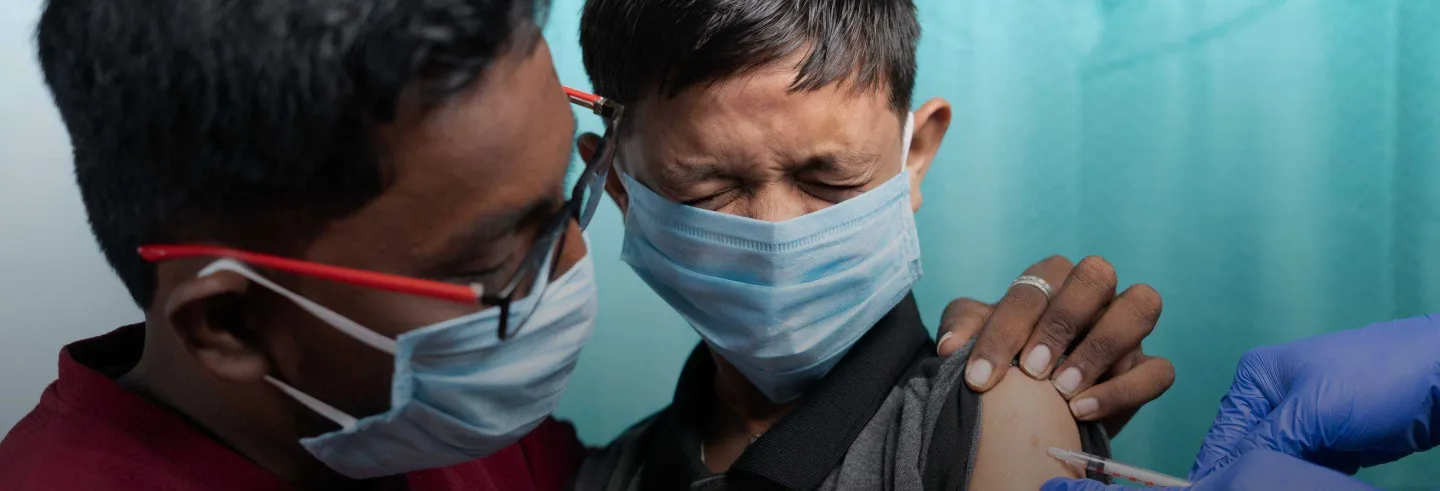
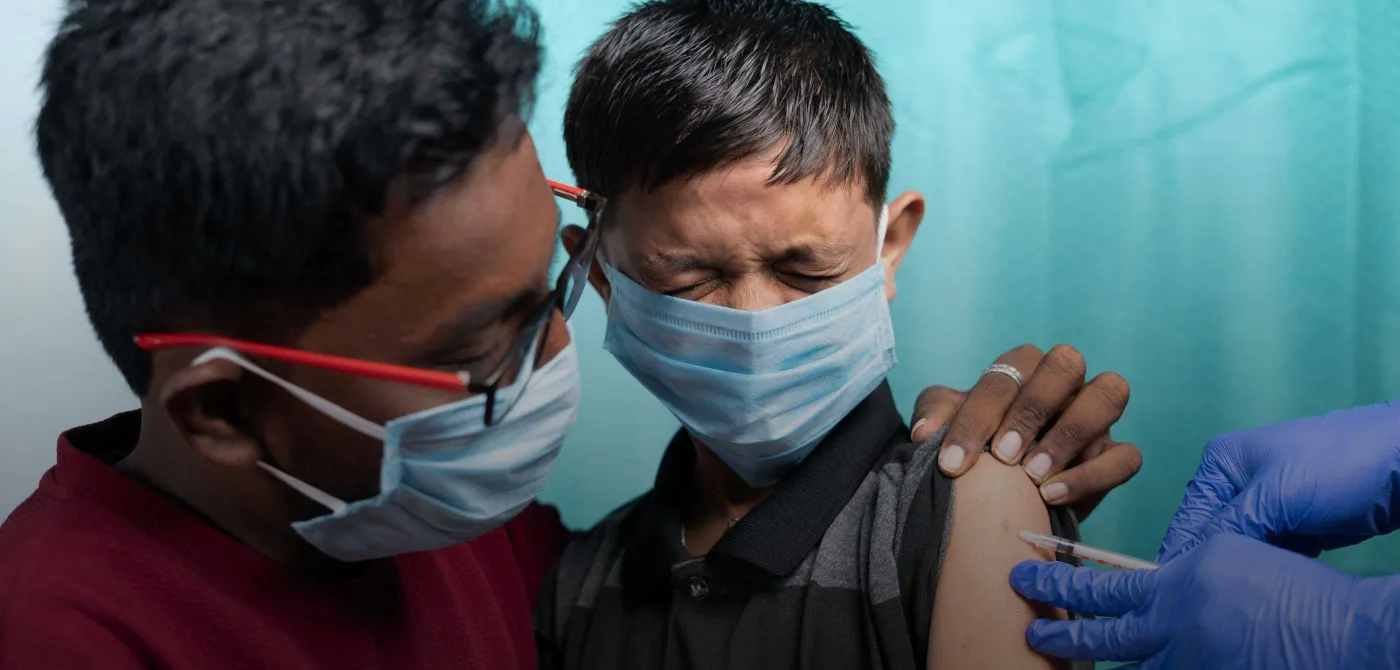
Over 30 countries are vaccinating children against Covid-19 with the mRNA vaccines, and at least four (Indonesia and Chile with Sinovac, and UAE and Bahrain with Sinopharm) with the Chinese inactivated vaccines.
What should India do and when? With which vaccine? In India, And now with the Omicron variant emerging, does that change the considerations of risk and benefit? ZyCoV-D, the DNA vaccine from Zydus Cadila has been approved for use in individuals 12 years and older, but while the government has placed an order it is not yet available and according to reports will be used in adults first. The Phase III trial included approximately 1,400 children between 12 and 17 years, making up about 5% of the total recruitment of over 28,000 participants. The interim analysis of 81 symptomatic RT-PCR positive cases showed an efficacy of 66%, based on 21 cases in the vaccinated compared to 60 cases in those who got a placebo, but there were no cases in children who received either vaccine or placebo. Immunogenicity data from children given ZyCoV-D are not yet available, but published data showed that eight of 10 adults given three doses of 2mg DNA, with four weeks between doses, made antibodies. Given the limited data in children, it makes sense for this vaccine to be used in adults first to build a larger safety, immunogenicity and effectiveness database before moving to children.
Covaxin, the inactivated vaccine from Bharat Biotech International, was evaluated in 528 children between 2 and 17 years of age and has been approved by the Drug Controller General of India (DCGI). The vaccine has received WHO Emergency Use Listing (EUL) for adults but not yet for children. Covovax, the protein subunit vaccine based on the Novavax vaccine is manufactured by Serum Institute of India and is being tested in 920 children between 2 and 17 years, while Corbevax, another kind of subunit vaccine made by Biological E is being tested in children above 5 years. Since the studies specifically of Indian children are all based on immune response rather than clinical efficacy, we should have the remaining results emerging in the next few months. If vaccines are immunogenic and efficacious in adults, they should be the same in children, but there are considerations of dosing and safety.
Making policy
When making policy, the importance of the quality and the quantity of evidence must be recognised, even as we understand that in a pandemic it may not always be feasible to have sufficient data at the time that decisions need to be made. Globally, many leading agencies, such as the World Health Organisation use the Grading of Recommendations, Assessment, Development and Evaluation (GRADE) tool for rating the quality of evidence (particularly for effectiveness) and the strength of recommendations. The tool is used to summarize evidence for practice guidelines and recommendations, health technology assessments and systematic reviews.
The US Centers for disease Control and Prevention, Atlanta, most recently used GRADE to make recommendation for the use of the Pfizer-BioNTech vaccine for children. Children from the ages of 5 to 11 in the US can receive two doses of a vaccine formulation that has one-third the dose given to adolescents and adults. The decision was based on a Phase II/III clinical trial that enrolled 2,268 children between 5 and 11 years who were randomized to two-thirds of the children receiving the vaccine and one third a placebo. With 3.3 months of follow up at the interim analysis, the vaccine prevented 90.9% (95% Confidence Interval 68.3%-98.3%) of symptomatic, laboratory confirmed Covid-19 in children with or without prior SARS-CoV2 infection (three vaccine recipients and 16 placebo recipients developed confirmed Covid-19, none were hospitalized). Further, the neutralizing antibodies developed by children in the trial were at least as high as the response in 16-25 year olds. A review of the burden of disease in children showed that Covid-19 was the eighth leading cause of deaths, that cumulatively 8,300 American children 5 to 11 years of age had been hospitalized, that this age group contributed 44% of the 5,217 cases of multisystem inflammatory syndrome in children (MIS-C) reported in the US.
Based on GRADE, the benefits of vaccinating 5-11 year olds for prevention of symptomatic COVID-19 was type 1 (high certainty), while potential serious side effects were type 4 (very low certainty) because of the small numbers and short follow-up, and type 2 (moderate certainty) for reactogenicity. Data on hospitalizations, deaths, prevention of MIS-C or prevention of asymptomatic infection were insufficient for assessment.
The UK Joint Committee on Vaccination and Immunisation (JCVI) has not yet recommended vaccines for younger children, but the UK Chief Medical Officers did in September 2021, recommend a single dose of the Pfizer vaccine to 12 to 15 year olds, stating that it believed that vaccination would help reduce transmission of Covid-19 in schools, possibly preventing school related outbreaks. The analysis by the JCVI had shown that a million first doses of vaccines would prevent 15.3 cases of MIS-C, 87 hospitalizations and 2.39 paediatric intensive care unit admissions. Based on these data, the JCVI continued to recommend vaccination of 16-17 year olds and a very generous list of co-morbidities for which younger children should be vaccinated, but not routine vaccination of younger children. The risk of myocarditis associated with the use of mRNA vaccines in younger age groups and the low risk of severe disease in younger children is a reason for the caution of the JCVI, but other advisory committees and governments faced with students needing to return to school have begun to vaccinate children.
We have very limited data on the burden of disease in children in India.
With Omicron, we know that the majority of infections reported with some demographic data, at least initially, indicate that it was infecting younger people 18-34 years of age, who were also less likely to be vaccinated. With all variants, if adults can be infected, children can be infected as well. However, at the moment, we have no idea how the Omicron story will play out in terms of transmission, escape from vaccine or infection-induced immunity or severity of disease. If transmission rates are very high and disease in any age group is severe, it will be important to vaccinate children to reduce exposure of the vulnerable to the virus. If transmission is high, and disease is mild or infections are largely asymptomatic, then the picture may not change very much from today. Without better data, it is not possible to understand the potential implications of Omicron for vaccination.
When vaccines are to be introduced into a national immunization programme, there are three critical considerations. First, the burden of disease, which considers the risk of infection, severe disease and death, which can be stratified by age, geography or risk group. Second, the performance of the vaccine, which considers safety, immune response and protection and the amount of disease expected to be alleviated by vaccination. Third, the programme readiness and the availability of resources and processes to be able to vaccinate target groups and sustain the programme.
The WHO has recently published an interim statement based on data reviews from the Strategic Advisory Group of Experts (SAGE) on Immunization and its Covid-19 Vaccines Working Group, and the Strategic and Technical Advisory Group of Experts (STAGE) on maternal, new-born, child, and adolescent health, and nutrition. From 2020 and until 25 October 2021, age disaggregated data available to the WHO showed that children under five years of age represented 2% of reported global cases and 0.1% of reported global deaths. Older children and younger adolescents (5 to 14 years) were 7% of reported global cases and 0.1% of reported global deaths, while older adolescents and young adults (15 to 24 years) represented 15% of reported global cases and 0.4% of reported global deaths. Deaths for all ages less than 25 years represented less than 0.5% of reported global deaths. Although children with co-morbidities experience severe disease, and children and adolescents can have prolonged clinical symptoms (known as “long Covid-19”) or rarely, MIS-C, overall, there are proportionally fewer symptomatic infections, and cases with severe disease and deaths from COVID-19 in children and adolescents, compared with older age groups.
Evidence from India
We have very limited data on the burden of disease in children in India. The most recent serosurvey conducted by the Indian Council for Medical Research in June and July 2021 included children for the first time and showed that more than half of children 6-17 years of age had been infected. Antibodies were found in 57.2% of 6-9 year olds and 61.6% of 10-17 year olds, indicating that over 280 million children have been infected. However, despite the huge number of infected children, we have very limited data on how many developed severe acute disease or MIS-C. There are only a few published studies from India on aspects of SARS-CoV2 infection, ranging from interactions with dengue to cytokine profiles in children with MIS-C. Anecdotal reports indicate that children who are hospitalized mainly had co-morbidities, but there have been healthy children who have developed severe disease and died. Media reports, discussions with paediatricians and single hospital figures do not add up to an understanding of what actually has happened in terms of infection, disease and deaths in children in India, and while the data may have been collected we have no publicly available information.
India is now well situated with regard to vaccine supply, but there continues to be a level of uncertainty about decision-making that is in the best interests of our children, our country and our world.
Similarly, while we do not have the mRNA vaccines with their risk of viral myocarditis, we have been using the adenovirus vectored vaccine in young adults and have many media reports of temporally related events that resemble thrombosis with thrombocytopenia syndrome (TTS), but the analysed data from the National Adverse Events Following Immunization Committee are limited to much fewer reports than expected. As an example, Sri Lanka reports TTS cases at higher levels than India, following immunization with the adenovirus vectored vaccine.
The WHO’s interim statement issued on 24 November 2021 reiterates its global goal of reaching 40% of each country’s population by end-2021 and 70% by mid-2022. It highlights the limited data from low- and middle-income countries (LMIC), but cited a review from January 2021 that showed that paediatric deaths per million children and case fatality rates were higher in LMICs than in high income countries (2.77 vs. 1.32 for deaths per million and 0.24% vs. 0.01%). It also stated that while younger children might transmit less well than adolescents and adults, it is clear that children are susceptible to infection and participate in transmission. The quantitative picture is less clear when comparing infection rates in different age groups, because of studies being conducted at different time points when different public health interventions were being implemented. For example, outbreaks have been reported from schools, camps and day centres, particularly when masks were not used or physical distancing not emphasized.
While the WHO’s interim statement recognises the direct health benefits of vaccinating children, it also points out that vaccination that decreases Covid transmission in this age group may reduce transmission from children and adolescents to older adults, and may help reduce the need for mitigation measures in schools, and that for the overall development of society, the importance of education and keeping children in school cannot be over-emphasized. Nonetheless, the WHO’s framework for operation is global equity and it states “as long as many parts of the world are facing extreme vaccine shortages, countries that have achieved high vaccine coverage in their high-risk populations should prioritize global sharing of Covid-19 vaccines through the COVAX facility before proceeding to vaccination of children and adolescents who are at low risk for severe disease.”
Based on where we are today, it is unclear that there is an urgency for vaccine introduction in Indian children beyond those with co-morbidities.
India is now well situated with regard to vaccine supply, but there continues to be a level of uncertainty about decision-making that is in the best interests of our children, our country and our world. With high seropositivity, limited data on severe disease in children with and without comorbidities and limited information on the safety of vaccines in use in India, how do we make decisions on whether to vaccinate children and which vaccine to use? With schools re-opening, parents worry about children and protecting them from infection. Yet, for the vaccination programme, despite the massive efforts and nearly 1.2 billion vaccines being given we still have a long way to go to vaccinate our adult population.
On vaccinating children
It is clear that children with co-morbidities need protection and if safe and effective vaccines are available, they should be used. ZyCoV-D has been evaluated and appears safe in children. Even with no cases in children, there is no reason to believe it will not protect in children as it does in adults, but immunogenicity data from children and a greater safety database in adults would be reassuring. Plans for introduction of any vaccine in children must be designed to monitor post-introduction safety in children, hopefully better than we have done in adults so far. For Covaxin, recent data on low protection against symptomatic infection in adults raises the question of vaccine effectiveness for prevention of disease, given that other inactivated vaccines have been shown to perform less well than mRNA or vectored vaccines in effectiveness studies. For Covishield which is not used in younger populations globally, no safety data are available for those under 18 years of age.
Based on where we are today, it is unclear that there is an urgency for vaccine introduction in Indian children beyond those with co-morbidities. There is, however, an urgent need to consider whether, similar to other parts of the world, we should be considering the use of one or two doses of mRNA vaccines. This would require the government to consider its policies for permitting the vaccines to be used in India as fully licensed or products which are approved for use during the pandemic with appropriate indemnification. There also needs to be consideration of strategies for introduction—school-based campaigns or routine immunization campaigns, all to be done without impacting a routine immunization that reached 90% of infants in its best year.
Even if programmatic readiness for introduction is not a concern, we need to recognise that the lacunae in the information on the burden of disease and the potential impact of vaccines in healthy children to be able to make an evidence or predictive modelling-based decision is a gap in our ability to deliver informed decision-making. There is an urgent need to strengthen our data systems to monitor both SARS-CoV2 infections in children and the safety, immunogenicity and effectiveness of vaccines, so that policy on vaccinating children is informed by evidence.