The onslaught of the Covid-19 pandemic has resulted in multiple outbreaks spread over a stretched-out period. Epidemiologists use the term “outbreak” when, resulting from a unique origin, there is an increase in the number of disease cases that spread among people. It is an increase in disease occurrence in a defined population that is "clearly in excess of the number of cases than usually or normally expected in that population". The increase in incidence can vary to qualify as an outbreak. A single case of anthrax or polio would be called an outbreak since we normally do not expect any such cases. For neonatal tetanus, two cases in the same hospital can constitute an outbreak in an area. In the case of Covid-19, several hundred or thousands of cases constitute a wave depending upon the geographical region and time period.
The meaning of ‘waves’
The standard English meaning of waves corresponds to that of a sudden occurrence of or increase in a phenomenon. In epidemiology it is not very different: a wave is an outbreak that can be defined as an upsurge in cases above the expected level during a defined time period. Each subsequent wave typically refers to a resurgence of a viral infection, with the wave characterized by increasing cases continually over a certain period in an area that had earlier witnessed transmission levels below the outbreak potential.
The duration of waves varies for different diseases. The seasonality of some enteric and respiratory viral diseases result in waves during the winter seasons. The seasonal wave of measles in India peaks in March, although it occurs throughout the year, with October-November being the low transmission months. According to the evidence, more than 68 infectious diseases are seasonal in nature, and the peak of the cases varies by seasonality in different regions.
The problem in identifying waves in India is that most of the states do not have robust surveillance systems...
In Covid-19, a simpler way of understanding a "wave" is that there are a large enough number of cases in a defined period of time that are sufficient to flag a public health concern and a response from the public health authorities.
The problem in identifying waves in India is that most of the states do not have robust surveillance systems and there is no clear way of understanding the expected number of cases of a disease. Therefore, it is difficult to explain the excess cases that do take place. Further, defining a clear population and time frame is needed for a clear definition. There are many areas where an outbreak has taken place that have not been noticed because of poor detection and real time data is rarely available in an accurate manner. There are also many areas with poor surveillance systems and are therefore outside the ambit of a population under observation.
While some countries have had distinct waves of Covid-19, a country like Brazil has had a perpetual wave (Figure1).
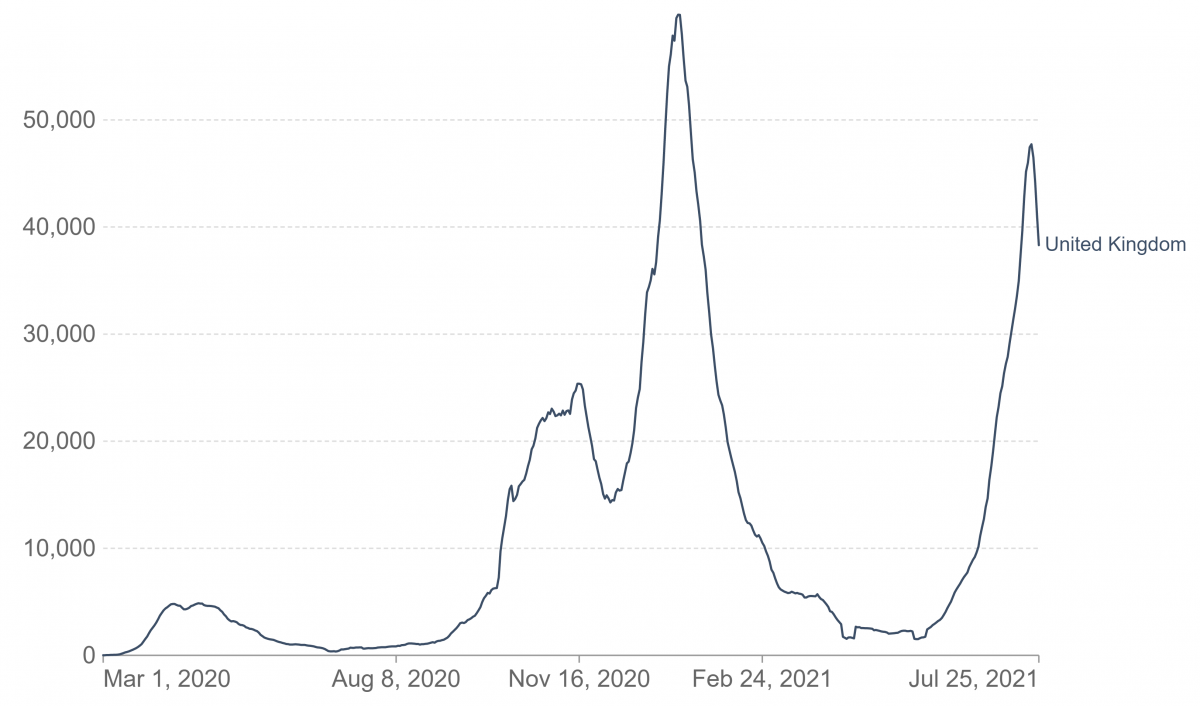
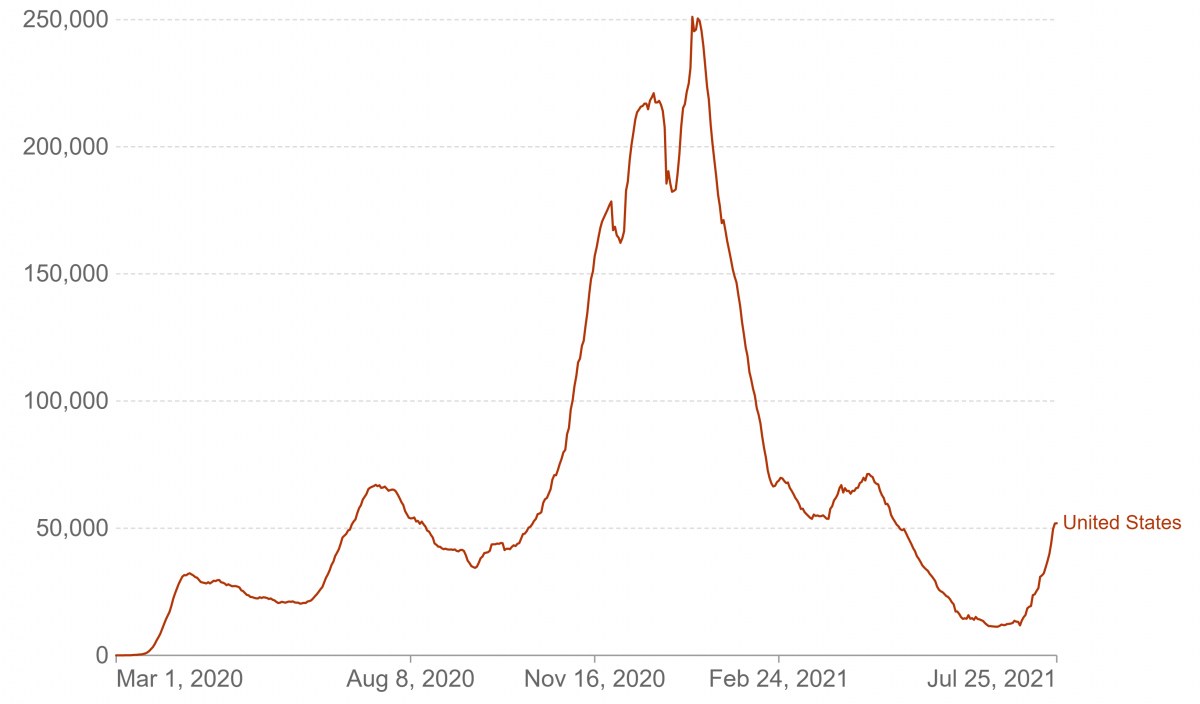
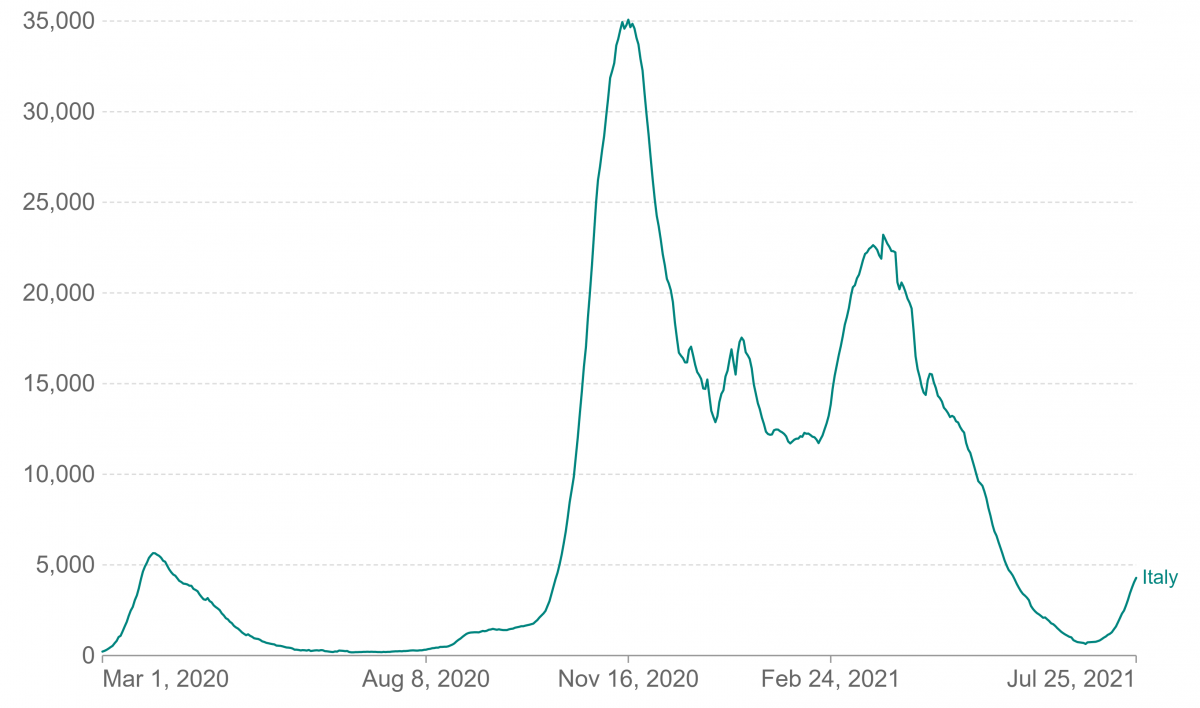
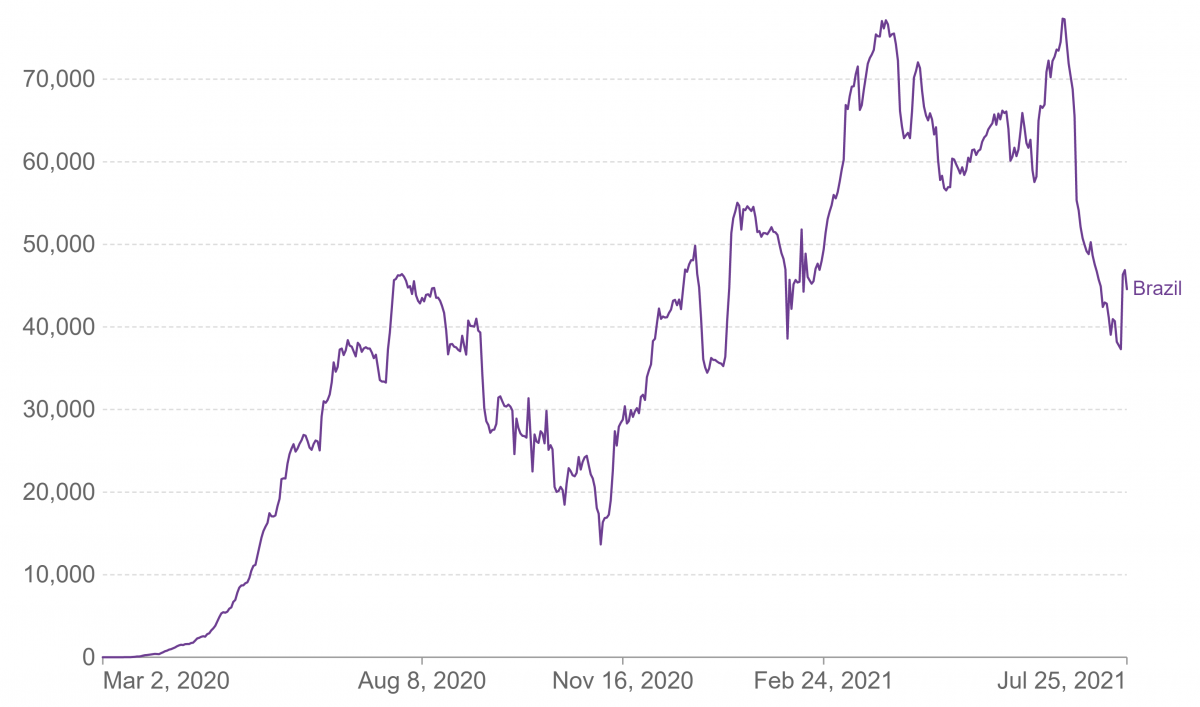
Identifying waves
There are several indicators to identify a Covid-19 wave. Identifying a potential wave is very active process and involves continuous monitoring of the disease trend.
The percentage of all coronavirus tests performed that are positive is referred to as the test positivity rate (TPR). A higher TPR indicates that either there is a higher prevalence of Covid-19 in the population, or fewer tests have been done, or both. When the seven-day TPR crossed 5, it is a trigger for action in containing the outbreak. An effective reproduction rate (R) above 1 or an increasing growth rate of deaths over seven days are also triggers for action.
Public health agencies use several ways to use these indicators to define a wave. For example, the occurrence of cases clearly in excess of normal expectancy can be indicated by the TPR doubling in a week, assuming there is no change in the testing pattern. Also, hospitalizations doubling in the corresponding seven consecutive days can also suggest the occurrence of a new wave. A wave is used to denote an upsurge in cases. The prerequisite conditions include that the earlier wave should have been contained (Effective R below 1), there then follows a low rate of infection sustained for at least a month or so, after which cases steadily increase over the next two to three weeks, crossing the reproduction rate of R=1.
For a wave to occur, an adequate pool of susceptible persons larger than a critical threshold level needs to build up.
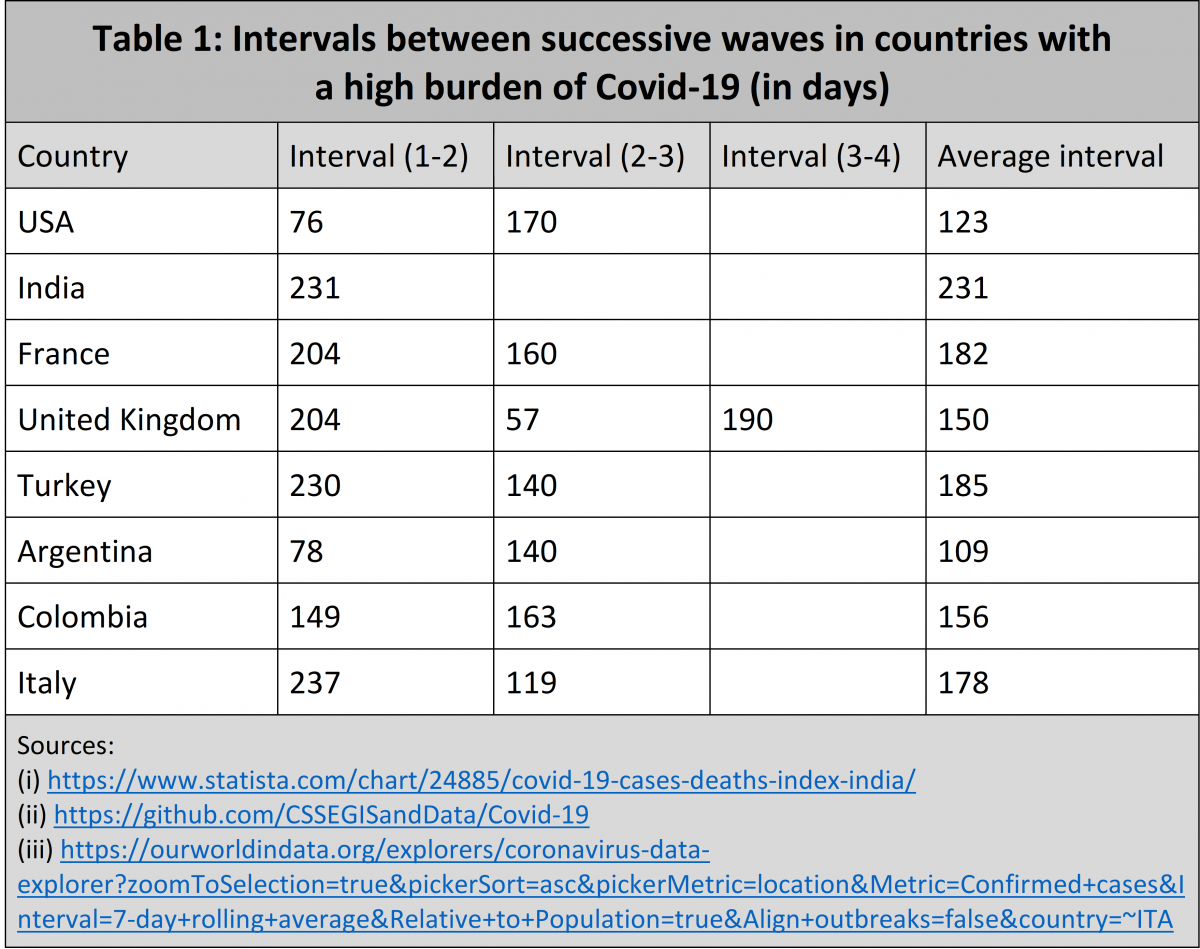
Considering waves in several countries (Table1 and Figure1), a wave is anticipated three to four months after the previous one. For a wave to occur, an adequate pool of susceptible persons larger than a critical threshold level needs to build up. This is facilitated by higher population movement, weak enforcements of Covid appropriate behaviour, a slower pace of vaccination, change in seasons etc. Not realizing this, earlier this year a major section of the media in India was reporting on political rallies and not focusing on the ground reality of the Covid crisis that was shaping up., This then led to the second wave.
Preventing waves, mitigating waves
Multiple factors lead to the formation of a susceptible pool of people and then to outbreaks.
In the Covid-19 pandemic, the main driver is the proportion of people who have not been infected so far and those who are not vaccinated. Seroprevalence surveys estimate the proportion of people having antibodies against the SARS-Cov-2 virus and, therefore, provide a reliable estimate about the total number of people who have been infected, including those infections that might not have been detected earlier. Efforts should be made to understand the seroprevalence at the sub-state level to identify areas with lower seroprevalence. These areas are at a higher risk in the next wave if prompt preventive actions are not taken. There is also a case for expanding the vaccination coverage in these areas so that the number of people who may require hospitalization and those who succumb to the infection are minimized if a new wave does take place.
Each subsequent wave of Covid-19 and its control will depend on the background prevalence of the infection. Areas with lower seroprevalence should have a special strategy. Next, concurrent genomic sequencing and epidemiological investigation of circulating variants should aid in preventing the spread of the virus. Whether or not there will be a wave in the future depends on how people adhere to public health measures. Typically, areas with low vaccination coverage will end up with a higher proportion of people with severe illness and deaths. Vaccination coverage should therefore be specifically targeted a at vulnerable areas; this will help lower the infection rate, especially in areas of high population density.
Waiting for the wave to hit without carrying out adequate surveillance is akin to seeking refuge in an open space amidst a hurricane. It is only strong disease surveillance that can thwart future waves. The rapid response teams at the district and subdistrict levels should identify and contain a cluster of cases. This should be done by strengthening testing, ensuring prompt contact tracing, and implementing community-based active surveillance for symptomatic cases. Surveillance for “Influenza Like Illness” (ILI) and “Severe Acute Respiratory Illness” (SARI) will yield sensitive indicators for picking up the transmission in early stages. At the same time, surveillance in closed settings such as schools/colleges, hostels, office spaces, prisons, long-term care facilities, hospitals, etc., should be strengthened.
Waiting for the wave to hit without carrying out adequate surveillance is akin to seeking refuge in an open space amidst a hurricane.
Irrespective of the Covid-19 variant and which wave it is, most of the public health responses must remain the same. Enforcing mask-wearing is necessary, especially in all settings where people congregate, and are the potential areas for spread of the infections. To mitigate the impact of future waves, non-essential congregations should be discouraged, and permissions delayed as much as possible in areas that could be badly affected. Mass gatherings within closed spaces (poor ventilation) should be actively discouraged. Preventing the formation of crowds is necessary, be it rallies, fairs, festivals, religious congregations, cultural events, etc. In the next few months, ahead of winter, all super spreader events should be prevented. Only a limited number of people should be allowed in congregations in closed spaces.
A whole of society approach is needed that includes every sector outside the government as well every department of the government. Such an approach can help the health systems in surveillance, contact tracing, admission of patients, earmarking of beds in private hospitals, etc. Microplanning and mobilization campaigns will also help avert or mitigate the impact of another wave. Non-pharmaceutical public health social measures (PHSMs), such as masking and physical distancing, should become a way of life.
The terminology of waves and how it is used in the media is at times confusing and can stigmatize active actions by public health authorities.
Government efforts are important but not complete without the participation of corporate organisations, NGOs and charity institutions in preventing future waves. Several mechanisms can be employed, such as Ward Decentralised Triage and Emergency Response Committees (DETER), led by citizen groups and civil societies. As Covid-19 cases are now again rising in India, these organizations should be engaged actively to explore ways and means for mitigating the adverse impact of future waves.
The terminology of waves and how it is used in the media is at times confusing and can stigmatize active actions by public health authorities. Usage of phrases such as “another deadly attack is here” can create fear about an impending lockdown. The usage of these terms is not preferred in epidemiology, but the description of waves in the mainstream media often feeds into the fear of people. While laypersons are looking for ways to make sense of what is happening, poorly crafted media messages can have extremes reactions, ranging from fear to apathy. Talk of an impending wave also reminds people of the past agony of fatalities and associated misery. Some media reports were responsible in 2020 for individuals fleeing from quarantine or isolation facilities and taking unnecessary travel prior to or during the lockdown to return to their homes.
An effective media communication strategy should be in place to allay fears and describe the epidemiological features in layperson language and form. These can include using sponsorships to organize (in regional languages) expert opinion shows, panel discussions to rope in role models (including popular personalities) to promote mask-wearing and preventing formation of crowds. The use of social media should be strengthened for clear and consistent messages also in regional languages. These messages should reinforce the need for Covid-19 appropriate behaviour at the population levels by engaging the public with the use of evidence-based information.
While laypersons are looking for ways to make sense of what is happening, poorly crafted media messages can have extremes reactions, ranging from fear to apathy.
Meanwhile, no hasty decisions to relax PHSMs should be taken. Every decision must take into account the risks and benefits to the community as a whole. How we deal with future waves of the pandemic will have a wide range of consequences for the health of society, the economy, mental health, psychosocial well-being, human rights, food security, and prevailing socio-economic disparities. Measures taken to prevent future waves or mitigate them(if they do happen) should avoid having an adverse impact on other public health programmes, treatment and management of chronic conditions other than Covid-19, and gender or age based violence.
Steps for preventing the next wave, or to mitigate it if does take place, should be based on evidence obtained through repeated serosurveys, assessment of vaccination coverage and evaluations of preparedness at the basic local administrative level. The available options should be administratively feasible, contextually relevant, and culturally appropriate in a coherent and coordinated way. Epidemiology is the main weapon to assess the ability of the health system to respond to the pandemic. In the assessing the timing and size of the next wave, epidemiology alone can guide a rapid decision-making process.
Steps for preventing the next wave, or if it does take place then to mitigate it, should be based on evidence obtained through repeated serosurveys, assessment of vaccination coverage...
The epidemiological indicators and their thresholds will determine the timing and size of another wave. These include the testing levels and distribution, data collection capability and utilization, micro plans for vaccination and social mobilization for coverage, and indicators for Covid-19 response. Markers of morbidity, mortality, and health-system pressure, such as occupancy of regular hospital beds and ICU beds are useful during the outbreak. But epidemiological data and analysis, namely, the effective reproduction number and the dispersion index (the clusters or number of infected persons identified by backward tracing) are needed to take decisions to prevent the onset of future waves or when they do set in, to mitigate their impact. Epidemic intelligence teams should support the district or state war rooms in recognizing the onset of the wave early on and in alerting the health authorities for quicker action.
Conclusions
In summary, although waves of a pandemic are not scientifically well defined, we do have knowledge of scientific actions that can prevent such events. If we follow evidence-based methods, we can both identify and prevent infection and loss of lives.
Acknowledgements: I thank Prafulla Shriyan, Aditi Deshpande and Hima Bindu Dubasi for their help with data pooling and proofreading.