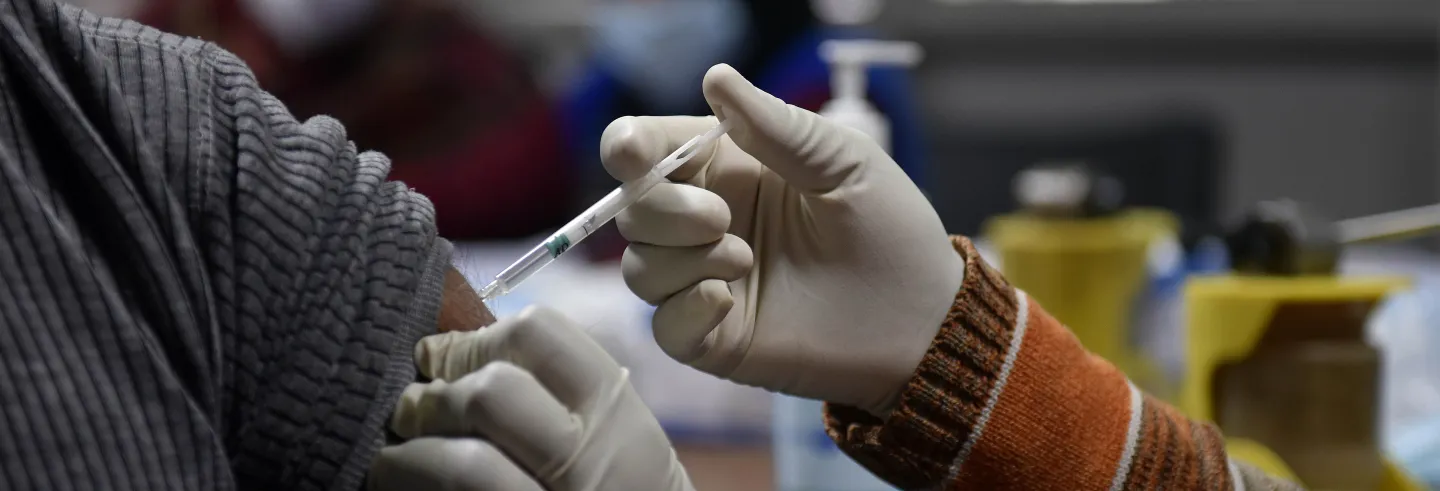
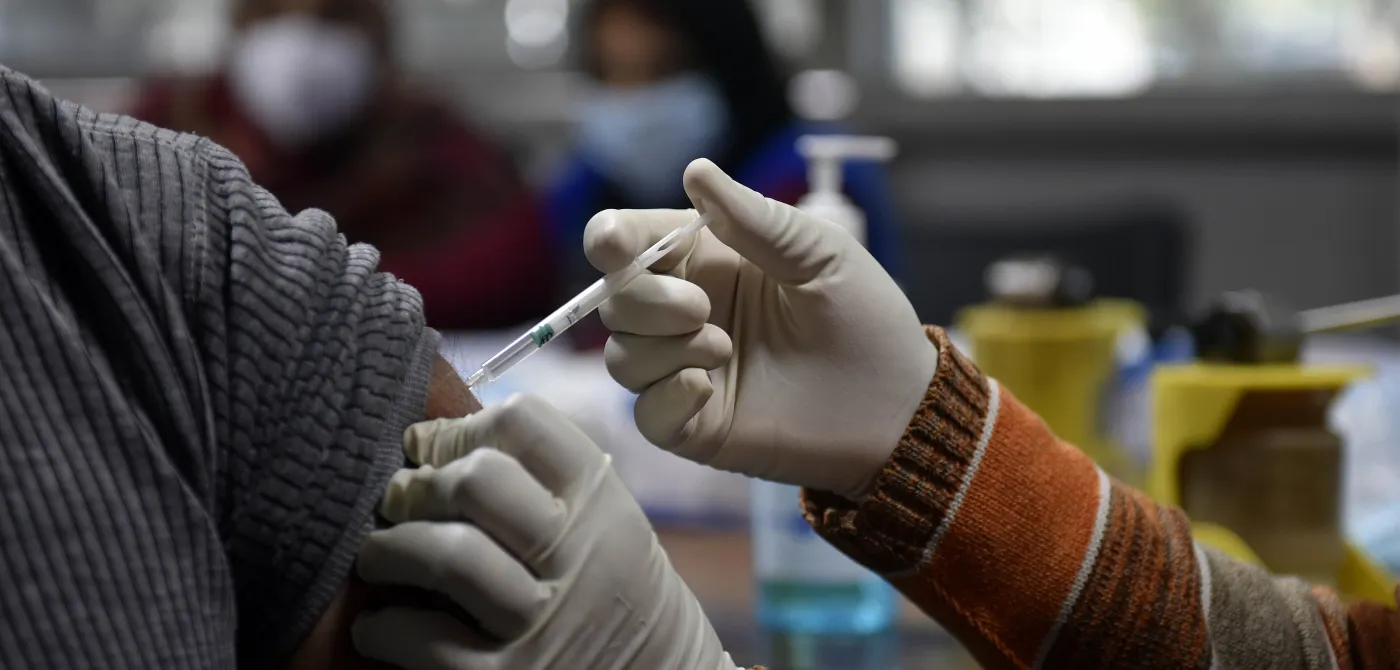
We have just passed a landmark in the Covid-19 pandemic. More people have been vaccinated against SARS-CoV2 than have been infected by SARS-CoV2. To a vaccinologist the explosion of vaccines being developed for SARS-CoV2 and the speed at which we have been able to move ahead, seems in some ways surreal. Vaccines have been available since the late 1790s and have traditionally been developed slowly, with great consideration at each stage of development.
We now have at least 10 vaccines in use in different parts of the world.
Pfizer-BioNTech’s and Moderna’s mRNA vaccines were first approved on the basis of clinical efficacy trials in the United States by the US Food Drugs Administration and subsequently approved under Emergency Use Listing by the World Health Organisation (WHO) and in several countries globally.
The second class of approved vaccines are the adenovirus vectored vaccines, including the Astra-Zeneca/University of Oxford vaccine, also made by the Serum Institute of India as Covishield, the Gamaleya Institute’s Sputnik V vaccine and CanSinoBio’s Convidecia. Efficacy data are available for the Astra-Zeneca vaccine, which vary depending on dose and interval from 53% to 90%, and for Gameleya’s vaccine which is 91% efficacious. Efficacy results are not yet available for the CanSinoBio vaccine.
Getting this far, this fast has been the result of immense, intense effort. It has meant compressing 10 years of vaccine development work into less than 10 months…
The third class of approved products are inactivated vaccines, for which clinical efficacy data are available for Sinopharm’s BBIBP CorV at 79%, and for Sinovac’s CoronaVac at just above 50% in Brazil and 65% in Indonesia, while efficacy data are awaited for Bharat Biotech’s Covaxin.
In the past week, high efficacy rates have also been reported from phase 3 trials for the Johnson & Johnson’s Janssen single dose vaccine and the Novavax protein vaccine, and it is expected that these will also receive emergency use authorization in the near future.
With the approval of the first vaccines for Covid-19, we have begun roll out programmes, perhaps not as fast as we would like but we are already ahead of where we predicted we would be at this time last year. Getting this far, this fast has been the result of immense, intense effort. It has meant compressing 10 years of vaccine development work into less than 10 months—an achievement that has only been possible because of science and the collaboration between academia, industry, policymakers and funding.
Despite all the advances we have made, there are still many important considerations for which we have no answers as yet.
Duration of protection
How long will vaccines protect? Because the vaccine trials were large, enrolling 20-45,000 participants in phase 3 studies in locations where case numbers were high, cases of disease accumulated quickly. This allowed a rapid comparison between those who were vaccinated and those who were not, proving quickly that the vaccines were able to protect against disease. But since all the successful trials so far have got their results within a few weeks to a few months after completing enrolment, we only have information on early protection. To understand how long protection will last we will have to continue to follow up the vaccinated people to identify ‘breakthrough’ infections that will show us lack of protection.
Protection against disease is a given for all successful vaccines, but some vaccines can also induce ‘sterilizing immunity’, where a vaccinated person cannot be infected.
Will vaccines protect only against illness or against the spread of disease as well? The primary outcome for phase 3 vaccine trials is protection against illness, but there are three outcomes for which vaccine efficacy can be studied. These are protection against disease, protection against infection, and effect on transmission or spread.
Protection against disease is a given for all successful vaccines, but some vaccines can also induce ‘sterilizing immunity’, where a vaccinated person cannot be infected. Sterilizing immunity is rare and unlikely for a pathogen that infects mucosal surfaces as in the respiratory system. But it is possible that while infection is not completely prevented, vaccines could reduce the amount of virus being shed, which could then lead to lower spread. There are early data from the Astra Zeneca vaccine showing decreased transmission. Such information is not available for the other vaccines. While it is likely that they will also have similar results, the early studies were not designed for testing participants regularly for virus shedding.
Protection against new strains
Will vaccines protect against new strains? In late December 2020, we had worrying laboratory data that indicated that SARS-CoV2 strains could evolve to evade the antibody response. It was not clear whether this would have immediate clinical significance, but data from the Janssen trial showed 72% efficacy in the US, 66% in Latin America and 57% in South Africa, while Novavax had 89% efficacy in the US and about 50% efficacy in South Africa. In the past few months, the B1.351 variant, also known as the 501Y.V2 has replaced older variants and has been shown in the laboratory to be less well neutralized by antibodies from people infected with the older viruses.
Does lower protection by some vaccines against the new variants mean that other kinds of vaccines will work better? It has been proposed that inactivated vaccines might be better against new variants than vaccines that are based on a single viral protein. This is feasible but unproven. The spike-based vaccines were developed because, based on the work with SARS-CoV and MERS-CoV, it was known that the spike protein was responsible for attachment and entry into cells during infection and blocking the spike with antibodies blocked infection. There are other viral proteins to which antibodies are made, but it is not known whether those antibodies or other cellular immune responses will be sufficient to protect from infections with variant strains.
Protection for those with a history of infection
Do vaccines protect as well or better than natural infections? Do people with a history of infection need to be vaccinated? In early vaccine trial results we have seen variable but generally high rates of protection, from 50% to 95%. There are also data that show that naturally infected people have more than 80% protection for at least five months.
While some protection from infection is expected, we have no way of knowing how good the protection is for each person, particularly because we do not know have an immune correlate of protection to see who is and is not protected. In some studies, up to 20% of people who had infection without symptoms had no antibodies, so a history of a positive test may not mean protection.
Based on this current state of knowledge, the WHO has recommended that people with a history of infection could delay their vaccination for a few months but should take the vaccine.
Strategy of vaccination
Over 10 million doses of vaccines have been given, and the roll out everywhere has been slower than planners and policymakers expected. This is only partially due to supply constraints. Despite awareness of timelines and logistic planning by governments, there have been numerous glitches ranging from unplanned storage requirements in the US to failures of the electronic app Co-WIN in India.
India was the fastest to reach 4 million vaccinated individuals, a promising start for a country with no adult vaccination programmes except for pregnant women. But there is a long way to go to reach the planned 300 million by August 2021—the current pace of immunization needs rapid amplification if timelines are not to slip further. Fortunately, lack of supply is not likely to affect India because the government had approved at risk manufacturing and both Covishield and Covaxin doses are available and ramp up of production is continuing.
Clear and transparent communication about what we know, and about what we do not know, are needed to build trust.
With efficacy results already available for three further vaccines, from Gamaleya, Janssen and Novavax, which have manufacturing agreements with Indian companies, we should have ample supply following technology transfer and bridging studies at different times during 2021. Further, the Zydus Cadila DNA vaccine is in phase 3 trials and other candidates, including the recombinant protein vaccine from Biological E and the RNA vaccine from Gennova, are starting clinical trials, further adding to the late stage Indian pipeline.
While supply might not be a constraint, we do need consideration of the strategy. At the moment, the government has rolled out a programme using a prioritization strategy for healthcare workers and essential workers, with those over 50 years of age and with other co-morbid conditions that place them at high risk of severe disease to follow. Will this be sufficient?
We have heard a lot about herd immunity, and the magic number of 60% or 70%. This refers to the expected slowdown of transmission, and therefore infections and disease, once a substantial proportion of the population is infected or vaccinated. But if a variant is more transmissible than the older versions of the virus, the percentage of people who must be protected needs to increase. If protection by vaccination or infection is short-lived, then again, the strategy for protecting the population will need to change.
We are also facing an epidemic of information, much accurate and much that is not. From untested treatments to immunity boosters to the dangers of vaccines, there has been both misinformation because people do not know better and disinformation where incorrect information is deliberately shared. Pseudoscientific information about vaccines contributing to sterility or causing placental damage or resulting in genetically modified humans have no basis in fact. But there are genuine concerns that people have about safety and efficacy, given that vaccines are given on a population scale to healthy people. Clear and transparent communication about what we know, and about what we do not know, are needed to build trust.
There is much that will be needed for the level and speed of coverage that is planned. Given the experience of the past few weeks, a re-orientation that includes immunization services being offered through channels other than the government seems advisable. For India, if we can scale the SARS-CoV2 programme with good immunization coverage countrywide, we should not treat this as a one and done approach but use the opportunity to build platforms for other adult vaccines, remembering that it is feasible that we may yet need boosters for SARS-CoV2.
Vaccines are giving us a way to look beyond where we are today, but vaccines are not the only tool we need.
India is fortunate in its vaccine industry, which has made access to vaccines at scale and reasonable cost possible for India and for the world. The government has already initiated vaccine diplomacy by gifting vaccines to several countries in the region and providing vaccine further afield. The numbers have been small so far, but will need to expand and rapidly, for supplies to the COVAX facility and to countries that have no manufacturers of their own. The COVAX facility is a multi-lateral undertaking where over 190 countries have banded together to buy vaccines together from manufacturers, thus leveraging their ability purchase large quantities, and using this approach to provide poorer countries with vaccines sufficient for about 20% of their populations. India expects to receive 97 million doses from COVAX and will hopefully be the major provider of vaccines. Chinese companies have begun to provide vaccines for COVAX. But as production increases and more products are licensed, India’s vaccine companies, which have provided much of the world with safe, efficacious and affordable vaccines for routine childhood immunization, will have the opportunity to be major players in the global supply chain of SARS-CoV2 vaccines.
Vaccines are giving us a way to look beyond where we are today, but vaccines are not the only tool we need. Numbers of cases have decreased dramatically in India without vaccines, and this is an opportunity for control that we should utilize. The principle of test, track and isolate are more easily implemented when case numbers are low, and are critical to preventing further spread and flare ups of disease in new areas or new populations. With good testing and tracking, we can be looking at how to open up schools, colleges, travel and economic activity.
Testing, drugs and vaccines are all the result of intense scientific effort and rigorous evaluation. On a score card, vaccines have done well, diagnostics reasonably and drugs not so well. With variants emerging, and limited drugs with proven efficacy, there is still a long way to go.