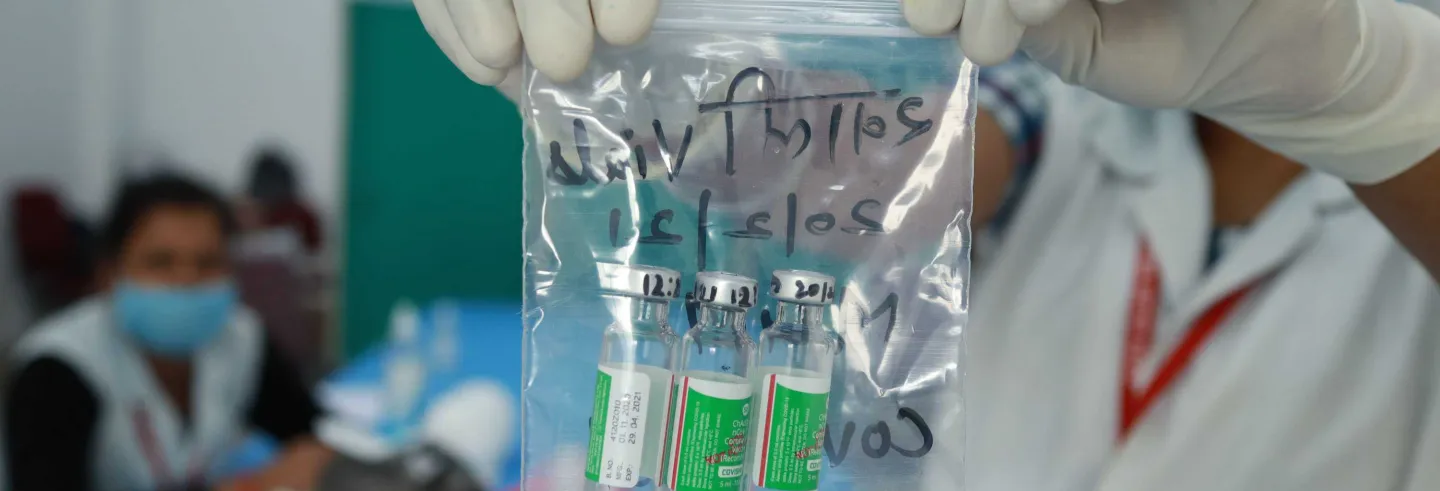
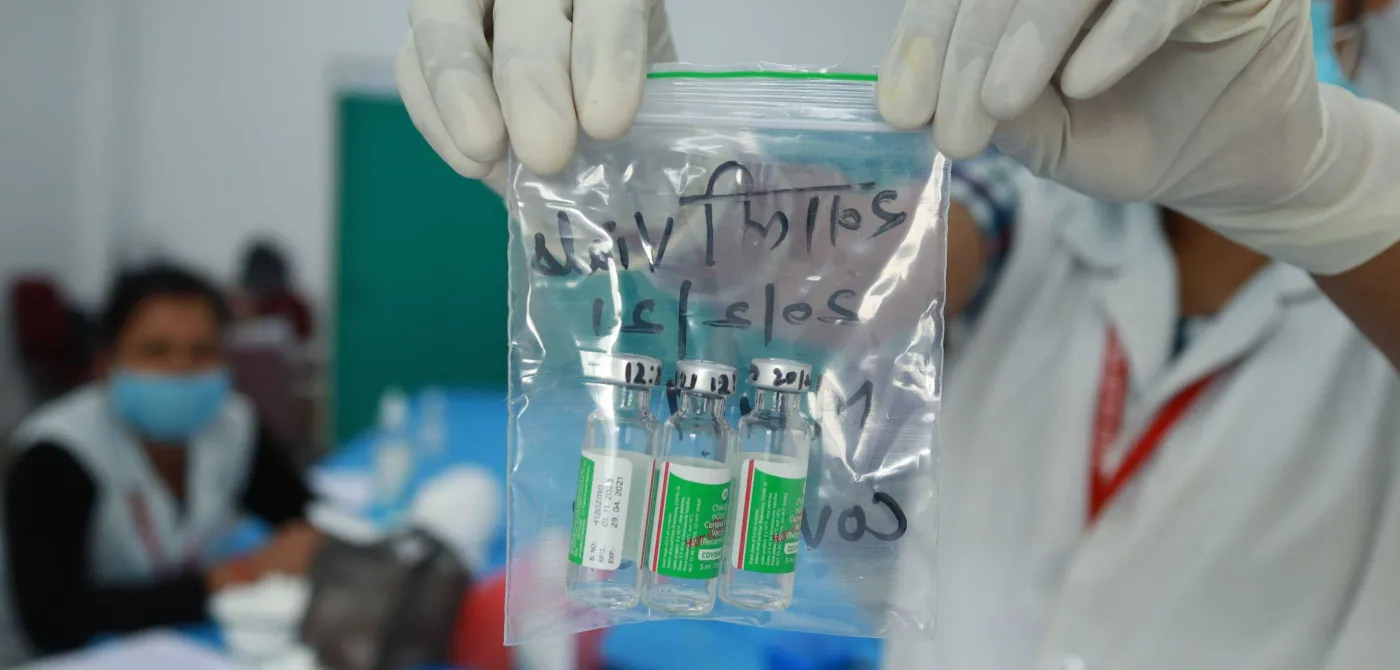
It is no small thing to immunise over a 100 million adults between January and mid-April in a country with poor health infrastructure and limited resources. But the pace of vaccination in India so far has not been rapid enough to blunt what could be a devastating second wave of the pandemic. And now vaccines are in short supply.
Numbers do not add up
The vaccine shortage was predictable. It has been clear for some time that the two manufacturers in India, Serum Institute of India and Bharat Biotech, were not going to be able to quickly meet the demand from the groups the government has prioritised for vaccination: those above the age of 45, as well as health care workers and others whose occupation puts them at increased risk. This is estimated to be around 400 million people and immunising them would require 800 million doses of vaccine, plus another 10% more to account for wastage. 1 Vaccine waste occurs because vaccines are bottled in vials of 10 doses or more, and at the end of a vaccination session, it is quite possible that doses are left over in a vial which has to be discarded. The government budgets for 10% waste when it allocates vaccine supplies.
The Serum Institute, based on statements made by its CEO, Adar Poonawala, produces around 60-65 million doses a month. Bharat Biotech is estimated to produce around 5 million doses a month, which is expected to double once a new manufacturing facility in Bengaluru is up and running in the summer.
The target of 800 million doses by August for 400 million people cannot be met with the existing manufacturing capacity in India.
At current production levels this amounts to between 65-70 million doses a month from both manufacturers. At this rate, from April to August, on a best case estimate around 350 million doses will be available to the government. If one adds the 80 million doses that had already been administered from January till 1 April, we get a figure of around 430 million doses from January to July. If we assume that Serum Institute can increase its production to 100 million doses by May (which it has been attempting to do for some time), this figure could go up to over 500 million doses by August. This is still well below the 800 million plus that will be required. The target of 800 million doses by August for 400 million people cannot be met with the existing manufacturing capacity in India.
Last year, while other major countries were either helping their manufacturers to expand production capacity to meet domestic needs (as China did) or funding vaccine manufacturers and making advance purchasing commitments as the United States, United Kingdom and many other countries were doing, India adopted a curiously laid back approach. The government encouraged Bharat Biotech to work with the Indian Council of Medical Research (ICMR) to develop a home-grown vaccine, but it was clear that this was not going to be enough to meet the country’s needs. Serum Institute had entered into sales agreements with Astra Zeneca and COVAX (the global vaccination distribution mechanism that had been set up by the World Health Organization and other international organisations), and it was assumed that at least half of Serum’s production would be reserved for Indian use.

But the government itself made no moves to indicate how many vaccines it would require. It was only in the first week of January that the government issued a purchase order for 45 million doses, followed by another order in March for 100 million doses. Orders were also placed with Bharat Biotech for amounts that are not publicly available but must be significantly smaller than the quantities from Serum Institute. It was clear that this volume of vaccines was not sufficient for the 400 million odd people who had been prioritised for vaccination.
The government’s strategy to make up the missing numbers was also never fully disclosed. Before the second wave started in earnest, vaccination numbers were small. Perhaps it was thought that demand would be so small that it would be possible to manage with existing capacity. Now, even with the government clamping down on exports, the numbers still do not add up.
Official pronouncements…seem primarily designed to create a portrait of Indian exceptionalism, infallibility, self-reliance and global leadership.
However, the government continues to maintain there is no shortage of vaccines. “Where does question of shortages arise? We are continuously monitoring and enhancing supply,” Union Health Minister Harsh Vardhan tweeted recently. This was despite photographs in the media of vaccine centres in several states displaying notices telling the public they had no stock.
A refusal to acknowledge any shortcomings has been a constant theme in government policy through the pandemic. Official pronouncements whether from ministers or from senior civil servants seem primarily designed to create a portrait of Indian exceptionalism, infallibility, self-reliance and global leadership. (“India has done better than other countries,” “India is the pharmacy of the world,” “The world is thankful to India for its vaccines.”)
The reality is somewhat different. India has the second highest number of Covid cases globally, and so has not done better than other countries. India might be the pharmacy of the world, but it is critically reliant on China for the ingredients that go into basic drugs. Countries that received vaccine shipments were grateful at first but are less so now that the government has clamped down on exports and prevented the Serum Institute from meetings its contractual obligations to COVAX, as well as to countries that had contracted directly with the company for vaccine supplies.
The Indian government did not play an active role in any of this, or finance Serum Institute for Covid vaccines.
Even the description of the Serum Institute’s Covishield vaccine as a ‘Made in India’ vaccine, while technically correct, does not convey the full truth. This is a vaccine that was developed at Oxford University with initial funding from CEPI, the Coalition for Epidemic Preparedness, an international group that funds research into pandemic vaccines. Astra Zeneca, the Anglo-Swedish pharmaceutical company, entered into an agreement with the Oxford group to manufacture and distribute the vaccine globally. Astra Zeneca in turn received funding from the UK and the US governments to help manufacture and test the vaccine in return for assured supplies. Astra Zeneca also received funding from COVAX to produce vaccines for poorer countries. Astra Zeneca in turn licenced Serum Institute to manufacture and distribute 1 billion doses of the vaccine to poor and middle-income countries, of which 400 million doses were to be delivered in 2021. Serum Institute received $ 300 million from the Gates Foundation and Gavi, an international vaccine alliance, to help it set up production facilities to meet its COVAX commitments.
The Indian government did not play an active role in any of this, or finance Serum Institute for Covid vaccines. Its only assistance was to remove regulatory hurdles and allow Serum Institute to manufacture and store the vaccine in 2020, before it was licenced for sale and distribution in the country.
Vaccine Maitri runs aground
The Vaccine Maitri campaign, under which over 64 million doses of vaccine have been distributed to 85 countries across the world has been portrayed in official statements (that the news media has repeated) as a government initiative to combat vaccine nationalism and provide global leadership in combating Covid-19. However, the bulk of these exports overseas are sales by the Serum Institute as part of its commitments to COVAX and Astra Zeneca. For the government to take credit for this makes no more sense than if it were to take credit for every export that any Indian company makes.
India is one of the few countries in the world that has actually donated vaccines to other countries: 10.5 million doses have been given…
At the same time, India is one of the few countries in the world that has actually donated vaccines to other countries: 10.5 million doses have been given to neighbouring countries as well as to countries in need in Africa and Latin America and the Caribbean. It can be argued that these donations, particularly in South Asia and Myanmar, were driven by the need to compete for influence with China. But this does not detract from the fact that people in these countries have received urgently needed vaccines. This is in contrast to the US, for example, which is sitting on stocks of 20 million doses of the Astra Zeneca vaccine that it is unlikely to use but is reluctant to give to countries in need. But creditable as India’s vaccine donations are, clubbing them with commercial sales by Serum Institute and Bharat Biotech to create the impression that the government was a major global vaccine supplier is to stretch the truth.
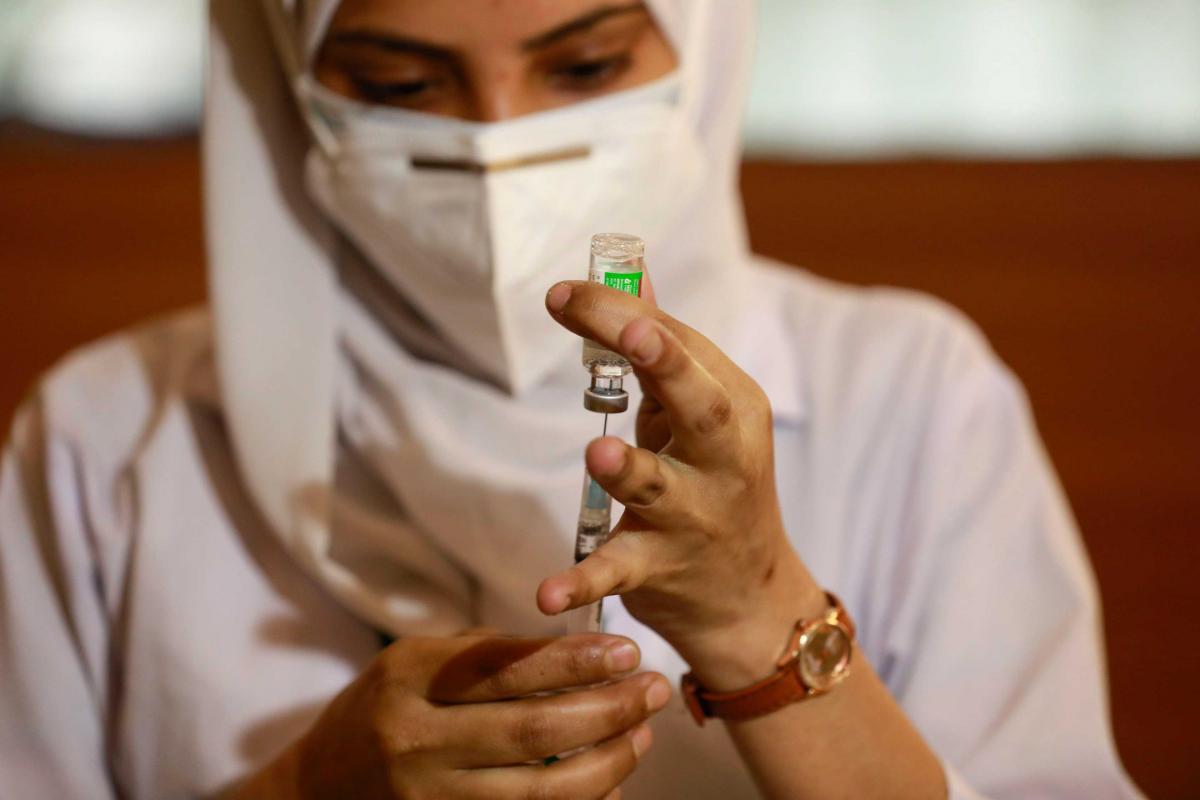
The rise of the second wave, the expansion of the domestic vaccination programme as well as the public backlash when it became known that more vaccine doses had been exported than used domestically, forced the government to stop exports. Serum Institute has had to stop its vaccine shipments overseas, defaulting on its commitment to provide 240 million doses of vaccine to COVAX by this summer. It has also reneged on agreements with Astra Zeneca whereby Serum Institute was to help Astra Zeneca fulfil some of its global vaccine supply commitments. Typically, the government has denied any ban has been imposed while at the same time preventing exports.
Countries in the neighbourhood that received gifts of vaccine and were planning to buy more from the Serum Institute, have suddenly found their vaccine supply drying up. Take Nepal. The Indian government donated 1 million doses of Covishield to Nepal, and the Nepalese government bought another 2 million doses from Serum Institute. Of the doses that it bought (and reportedly paid for at least partially in advance) only 1 million had been delivered by Serum Institute before India stopped exports. This has led Nepal to delay second doses for those who received their first dose, and to put on hold its plans to expand vaccination to cover younger age groups. It has also opened the door for China to export vaccines to Nepal, which bought 500,000 doses of the Sinopharm vaccine to restart its vaccination programme.
If India had hoped to emerge as a leader in global vaccine supplies, the abrupt reversal of policy is unlikely to have helped build the country’s reputation…
The stopping of exports has also brought supplies to poorer countries under the COVAX programme, for which the Serum Institute is the major supplier, to a halt. If India had hoped to emerge as a leader in global vaccine supplies, the abrupt reversal of policy is unlikely to have helped build the country’s reputation as a source of vaccines that could be relied upon.
Moving away from ‘aatmanirbhar’
The reality of vaccine shortages has also forced the government to step back from its ‘aatmanirbhar’, or self-reliance policy.
As has happened in earlier decades, Russia might provide a lifeline to India’s vaccination campaign. Last August, Russian authorities approached India about selling its Sputnik V vaccine in the country and also using Indian companies as a base for global exports.
In September 2020, Dr Reddy’s Laboratories and RDIF, Russia’s sovereign wealth fund which has invested in Sputnik V, announced an agreement to sell 100 million doses of the vaccine in India, once Dr Reddy’s had organised the bridging clinical trial required by the Drugs Controller General of India before the vaccine could be authorised for emergency use.
No results of these trials have been disclosed, but on 13 April the vaccine was given emergency approval, increasing vaccine supplies by 100 million doses, provided the government could agree on a price at which it would buy the vaccine.
India has now rolled out that welcome carpet for vaccine manufacturers across the world. But it is not at all clear whether this will have any immediate impact on vaccine supplies…
If the potential arrival of Sputnik V marked a move away from the aatmanirbhar policy, a second, even more abrupt move was made when, on the same day, the Drugs Controller General of India did away with the provision that foreign vaccine manufacturers had to conduct bridging trials in India before being allowed to market their products. While the requirement for trials was not done away with, this could be done after the vaccines were used in India (though it was not clear how this was to be actually achieved).
VK Paul a key figure in government vaccine policy, was quoted in news reports as saying that if regulators in the US, UK, Europe, Japan or the WHO had cleared the vaccine for emergency use, it could be used in India. “We hope and we invite vaccine manufacturers such as Pfizer, Moderna and Johnson and Johnson and others to be ready to come to India at the earliest,” he said.
This is in contrast to the government’s policy earlier in the year when Pfizer applied for authorisation to market its vaccine in India. The Drugs Controller General at that point said Pfizer needed to do trials in India before approval, something the manufacturer was not willing to do.
India has now rolled out that welcome carpet for vaccine manufacturers across the world. But it is not at all clear whether this will have any immediate impact on vaccine supplies in the country. Global vaccine supplies are extremely tight, and there is a waiting list. The European Union and UK are squabbling over supplies of the Astra Zeneca vaccine. The only supplies that are likely in the near term for India are of Sputnik V, provided the government can get it at a price it can afford. Officials maintain that funding for vaccine purchases is not an issue. But it clearly will be an issue. And the government does not have the kind of leverage over the Russian government that it has over Serum Institute, an Indian manufacturer.
Conclusions
Had the government planned for the possibility of a second wave and thought of ways to mitigate the surge in infections, it would have speeded up the roll out of vaccines beginning in January. It could then have taken policy measures to increase supplies, either from overseas or by encouraging more players, including in the public sector, to start production.
Postscript
The figure of 5 million doses a month production by Bharat Biotech in this report was an under-estimate based on the then available figures. Dr Krishna Ella of Bharat Biotech has since spoken in public of raising monthly capacity from 10 million to up to 60 million doses (700 million doses a year) by the end of summer. However this still does not close the gap between vaccine supply and demand.