The Covid-19 pandemic has brought about unique challenges for governments and public health authorities across the world. It has also provided them with exceptional legal and judicial powers to restrict and control people’s lives and livelihoods. But while the virus may be new, the modes of its control and prevention are not. Key aspects of the outbreak of Covid-19 and the measures to control it have historical and colonial legacies. Although the lockdown and the restrictions on public life in India appear unprecedented, they reproduce measures that colonial governments and public health officials had used to segregate, isolate, and confine people during epidemics.
These measures include the legal provisions used for control, the development of experimental vaccines, the tracing of the asymptomatic carriers, the asymmetrical social and economic consequences, and the violation of basic human rights, particularly those of the poor and marginalised communities. Historically, governments have sought to deal with largescale epidemic outbreaks through isolation and vaccination, both of which are at play in dealing with Covid-19. The extraordinary powers assumed by governments to undertake this twin task raise questions of ethics, human rights, and the use of state powers over the lives and bodies of its citizens.
Colonialism provided the first model of using scientific means of pandemic control for the large-scale and often coercive regulation of people’s lives and livelihoods [...] In times of crisis, postcolonial governments, health officials, and privileged citizens keep returning to these familiar patterns of self-preservation.
The instances of pandemic control in South Asia in the colonial past are vital to revisit. They illustrate the precedents of how political and social power operates in such times. Colonialism provided the first model of using scientific means of pandemic control for the large-scale and often coercive regulation of people’s lives and livelihoods. This model has been useful for states in the current crisis. In times of crisis, postcolonial governments, health officials, and privileged citizens keep returning to these familiar patterns of self-preservation, which often add to the suffering of the most vulnerable.
The colonial mould
In imposing the strict restrictions of the lockdown for Covid-19, the Indian government invoked the very same Epidemic Diseases Act of 1897, originally passed by the British government during plague outbreaks. This was a unique act, designed specifically to control an epidemic outbreak, giving special powers to the state, which is partly why it has appeared relevant for Covid-19.
The outbreak of the plague epidemic in Bombay in 1896 fundamentally changed the relationship between the colonial state and its subjects. This was the first instance when the state acquired special legal and judicial powers for an apparently humanitarian cause: to prevent the spread of the epidemic. To do so, it specifically targeted the poor and the migrant workers, seen as the carriers of the disease, restricting their movements, demolishing their homes, and subjecting their bodies to medical experiments. This became the model for subsequent governments to use disease or epidemics to justify authoritarian measures, all the way into the current pandemic.
The colonial authorities [had] almost unrestricted power to restrict the movements of the poor, migrant workers, and Muslim pilgrims. [Such measures] continued to be the mainstay of the colonial state's anti-plague campaign well into the first part of the twentieth century
The Epidemic Diseases Act gave the colonial government the right to inspect and isolate anyone suspected of being infected with plague, in public places, trains, ships and inside their homes. It simultaneously protected the state or the government officials from any legal action while acting under the act. Prior to this, the colonial government had in 1895 introduced the Pilgrim Ships Act to control the movement of Haj pilgrims from South Asia on health grounds. This gave local authorities in India new powers to board the pilgrim ships at any time to carry out inspections and apprehend any passenger in the name of disease prevention. The two acts combined to provide the colonial authorities almost unrestricted power to restrict the movements of the poor, migrant workers, and Muslim pilgrims.
The act was used in large parts of the plague-affected localities of Bombay and Pune, to demolish dwellings and clear the cities of so-called ‘vagrants’, beggars, and migrant labourers. These measures continued to be the mainstay of the colonial state's anti-plague campaign well into the first part of the twentieth century. The government used the acts to prohibit immigration from India, particularly from the infected areas; to to suspend railway travel to certain areas, and to obstruct of the pilgrimage to Mecca. After the plagues ceased, the Epidemic Diseases Act was employed rarely, perhaps because there were few such sudden pandemic outbreaks.
Vaccination by trials
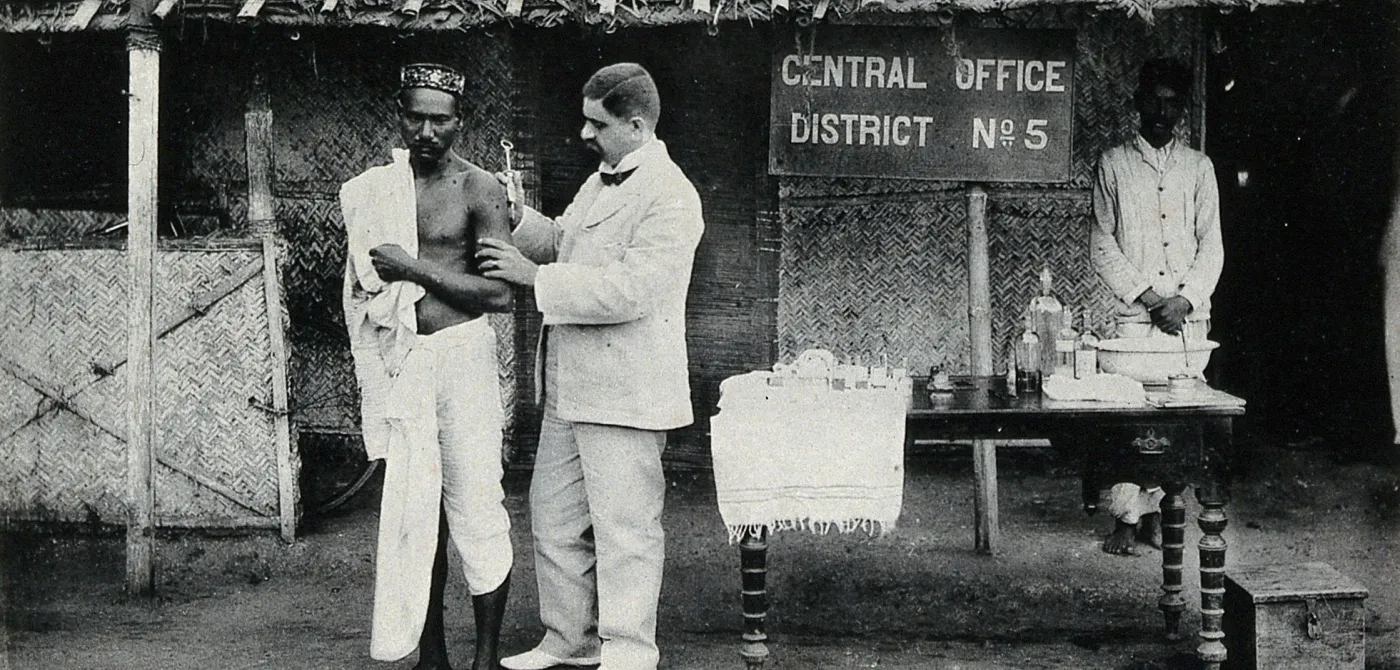
The Bombay plague provided the opportunity for public health officials and scientists for the production and the large-scale experimentation of vaccines in the colonies. Just a decade before the outbreak, the French microbiologist Louis Pasteur had created the first attenuated vaccine for the rabies virus. This created the possibility that all viral and bacterial diseases could be prevented by similarly developed vaccines.
Bombay, with its vast and diverse population and confined spaces such as jails, hospitals, and slums, became the ideal site for experimenting with these vaccines.
When plague broke out in the 1890s, the bacteriologists Alexandre Yersin and Shibasaburo Kitasato had independently announced the isolation of the plague bacillus in Paris and in Hong Kong, respectively. With the outbreak of the plague, scientists developed competing vaccines, similar to the present day global rush to produce vaccines for Covid-19 and to conduct human trials. In India, the Russian-Jewish scientist Waldemar Haffkine prepared his own plague vaccines in a small lab in Bombay..
Bombay, with its vast and diverse population and confined spaces such as jails, hospitals, and slums, became the ideal site for experimenting with these vaccines. During the outbreak, colonial medical officials experimentally injected residents with at least six different types of vaccines. European bacteriologists such as A. Lustig, Yersin, Paul-Louis Simond saw Bombay as the perfect laboratory for their vaccines and visited the city to observe the experiments. The authorities carefully selected groups of communities as samples for the experiment with the respective vaccines. These vaccinations were not designed to introduce any immunity against plague among the population but were carried out as ‘trials’ for these vaccines (Chakrabarti 2012, 49–55). There is no evidence that any kind of consent was ever sought for these experiments. While the colonial government did not introduce any legal protection for those being vaccinated, even experimentally, it introduced laws to enforce vaccination.
These colonial measures were part of a trend in the 19th century where governments across the world assumed greater legal powers to conduct large-scale vaccination. Smallpox vaccinations were made compulsory in various parts of the world. Beginning in 1853 in the United Kingdom, it was soon applied in the colonies. The outbreaks of smallpox in 1865 in Calcutta, in 1876 in Bombay, and in 1884 in Madras led the provincial governments to introduce Compulsory Vaccination Acts in these Presidencies.
Gaps in legal provision ensured that human subjects in colonial India had little control over their bodies in the pandemic state. These trends continue into the postcolonial state.
The coercive nature of vaccination has left a strong legacy of anti-vaccination campaigns and protests. Throughout Europe and North America, opponents regarded vaccination as threats to their health as well as an invasion of their rights. They formed anti-vaccination leagues, demanded that the government abolish compulsory vaccination, rioted, forged vaccination certificates, staged boycotts, and hid sick children. In India, the persistence of the arm-to-arm method, in which children, often belonging to lower castes, were used as carriers of the lymph for vaccination, was a matter of fierce public debate and resistance.
The debates have been on whether rights of individuals are greater than that of the welfare of the larger collective. As and when vaccines, prophylactics, or drugs become available for Covid-19, there will be questions of how these can be made acceptable and accessible to large sections of the population. Historically, mass vaccinations and drug trials, particularly of those at early stages of their development, are as beset with abuse of human rights as with the exercise of state power. Gaps in legal provision ensured that human subjects in colonial India had little control over their bodies in the pandemic state.
These trends continue into the postcolonial state, with state governments and public health authorities recommending the use of unproven hydroxychloroquine as a prophylactic against Covid-19 for slumdwellers, police, and other frontline healthworkers, including those in present day Mumbai. The recent controversy on the Indian Council for Medical Research’s rush to produce a vaccine for Covid-19 by Independence Day on 15 August 15, which has been deemed unfeasible by many experts, highlights that vaccine production timetables have deeply political mandates. With the decision to cut out some of the unnecessary ‘red tape’, questions of the safety and efficacy of the vaccine, whenever it is available, will remain important.
Symptoms of the asymptomatic carrier
Identifying asymptomatic carriers, individuals who do not show any symptoms yet carry the pathogens in their bodies and are capable of infecting others, is a significant part of any preventive strategy for Covid-19. When millions of Indians might never be tested for the virus or its antibodies how will we establish who is an asymptomatic carrier? In the absence of scientific proof, the question often is: who appears to be symptomatic?
Prejudices about class, gender and caste address this question. In India, the scientific idea of ‘asymptomatic carrier’ is introducing new forms of ‘untouchability’. Upper caste and class Indians are seeking to distance themselves from the poor, Muslims, and lower castes, whom they perceive as the carriers of the virus. There have been reports in India of migrant workers being sprayed with chemical disinfectants, of several of them are restricted from returning to their home while facing starvation due to the lack of work, and of international travellers and visitors being assaulted by vigilantes.
Koch’s scientific thesis of the asymptomatic carrier provided seeming validity to the entrenched layers of cultural, social, caste, racial, and nationalist prejudice in South Asia.
The idea of the asymptomatic carrier was proposed by Robert Koch in 1902, when he suggested that healthy individuals, who show no signs of a disease, could carry within them germs with which others may be infected. Long before this discovery, certain communities had historically been seen as likely carriers of disease. Koch’s scientific thesis of the asymptomatic carrier provided seeming validity to the entrenched layers of cultural, social, caste, racial, and nationalist prejudice in South Asia.
This has contributed to government actions against individuals or groups perceived as disease carriers and towards upper-caste communities segregating themselves even further from the lower castes and the poor. In colonial India, the British widely regarded poor and working-class Indians as carriers of multiple diseases. As with the poor residents of Bombay in the time of plague, in times of the coronavirus, some groups continue to be presumed infected before proven.
The scientism of the so-called ‘carrier-state’ theory has become a tool to legitimise major and often prejudicial global and colonial immigration control and segregation policies. Twinning quarantine and immigration, authorities often identified certain groups as potential ‘carriers’ of diseases and subjected. Jews, Irish, Mexicans, Haj pilgrims from South Asia, and the Chinese were at various times in the past subject to rigorous medical checks or to lengthy quarantine at immigration points, and even barred from entering specific countries. To do so, authorities sometimes used existing legal provisions or created new ones.
The strict lockdown measures for Covid-19 needs to be seen alongside the general disinvestment in public health and the poor medical facilities available for the vast majority of the population. It is usually easier to establish quarantine measures than to build preventative healthcare.
The incidence of quarantine against Ebola during its outbreak in western Africa in 2014-15 and the restrictions imposed in the United States on travel from that region shows how the question of the asymptomatic carrier and quarantine remain. In a notable case Kaci Hickox, an American nurse treating Ebola patients in Sierra Leone was quarantined on her return. Research showed that the very low risk of Ebola transmission from asymptomatic individuals and that quarantines of asymptomatic individuals with potential Ebola exposure were unnecessary. In the ensuing legal case, the court declared that quarantine of Hickox was not necessary since the evidence supported that asymptomatic persons were not infectious.
Conclusions
The resurrection of the Epidemic Diseases Act for Covid-19 reflects colonial modes of drastic governmental action, which has once again exposed the most vulnerable communities to greater health and economic risks. The strict lockdown measures for Covid-19 needs to be seen alongside the general disinvestment in public health and the poor medical facilities available for the vast majority of the population. It is usually easier to establish quarantine measures than to build preventative healthcare. While the colonial government introduced strict quarantine, it did not invest similarly in public health.
The colonial past provides important lessons of how pandemic outbreaks have not only caused huge mortalities but have also sanctioned extreme governmental powers.
In contemporary India as well, the lockdown is accompanied by an acute shortage of doctors, nurses, hospital beds, and other medical infrastructure. In these lockdowns in contemporary India, in the millions of poor people suffering without food, income, shelter, and adequate healthcare, colonialism is finding new forms of expression. As we deal with the current outbreak, we are also faced with the question of what Covid-19 will leave behind.
While on the one hand there is the possibility of more such outbreaks taking place, there is also the prospect of greater social and political control of our lives becoming the norm. While we prepare ourselves for and take precautions against similar such outbreaks in the future, we need to simultaneously raise questions of liberty and freedom associated with such provisions. The colonial past provides important lessons of how pandemic outbreaks have not only caused huge mortalities but have also sanctioned extreme governmental powers.
In the case of the Covid-19, the impetus for such control has come not just from the Indian state. Society itself has sought to be governed at a much wider and deeper level. Several of the strong governmental actions enjoy support from large sections of the population. Among certain sections, the popularity of government has reportedly soared because of the drastic lockdown measures it has taken. Bill Gates praised the Indian government’s strong and ‘proactive’ actions against the outbreak, even as numerous migrant workers were stranded without food, money or any means of travelling or earning their livelihood.
For India, Covid-19 might imply that certain populations will be faced with long-term and stricter regimes of social control and exclusion, while their labour is extracted from a distance.
What is the humanitarian position here, imposing more restrictions on people’s lives or alternatively allowing them to make their choices? We are clearly seeking more governance or more precisely stronger state intervention than ever before. Is that choice, both in India and elsewhere, being made by certain sections of the society at the expense of others? For India, Covid-19 might imply that certain populations will be faced with long-term and stricter regimes of social control and exclusion, while their labour is extracted from a distance. Covid-19 has made the return of the spectre of colonialism more real.